
Randomized controlled trials have not demonstrated any clear difference in mortality when comparing rate and rhythm control. Rate control does not affect the rhythm per se. Rhythm control, on the other hand, attempts to restore sinus rhythm by use of antiarrhythmic drugs. Rate control implies the use of medications that slow ventricular rate (beta-blockers being the mainstay of this therapy). Besides anticoagulation, atrial fibrillation is treated with rate and/or rhythm control. Wrfarin and novel oral anticoagulants can reduce the risk of stroke by 70%, as compared with placebo. Treatment with anticoagulation is highly effective in reducing stroke risk. This is not surprising given the adverse effects of long periods of tachycardia and desynchronized atrial and ventricular activity.įortunately, the treatment of atrial fibrillation has come a long way. However, the increased risk in mortality is not completely explained by the increased risk of stroke people with atrial fibrillation are at increased risk of cardiovascular mortality in general. Such thrombi may leave the appendage and enter the systemic circulation which causes thromboembolic occlusions of arteries in the brain, limbs or other organs. The increased risk of stroke is explained by formation of thrombi in the left atrial appendage. In multivariable models (i.e statistical models in which adjustment has been made for confounders) individuals with atrial fibrillation are at five times increased risk of stroke and two times increased mortality, as compared with individuals without atrial fibrillation. Complications of atrial fibrillation and available treatments Atrial fibrillation in other circumstances (particularly those listed above) is usually a progressive disease.Īll clinically relevant aspects of atrial fibrillation – from risk factors, complications, electrophysiological mechanisms, ECG interpretation to management – are discussed in this chapter.
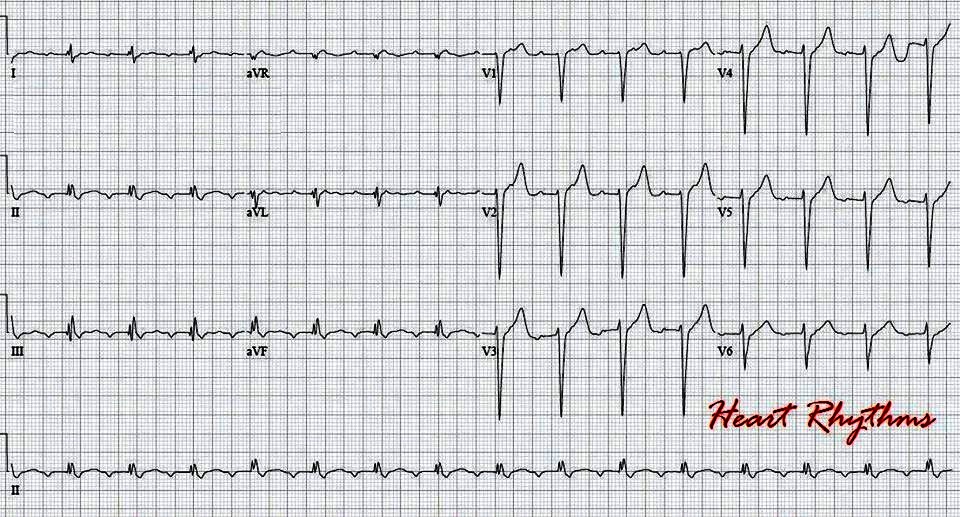
Moreover, certain other tachyarrhythmias predispose to developing atrial fibrillation: atrial flutter, AVNRT and AVRT (pre-excitation, WPW syndrome) being the most common.Ītrial fibrillation with onset during hyperthyroidism (thyrotoxicosis), alcohol overdose, thoracic surgery, acute myocardial infarction, pericarditis / myocarditis or pulmonary embolism is often a reversible arrhythmia with low risk of recurrence. Indeed, the strongest risk factor for developing atrial fibrillation is age. Other significant risk factors are as follows: male sex, hypertension, left ventricular hypertrophy, left ventricular dysfunction, valve disease, coronary artery disease, cardiomyopathy, congestive heart failure, congenital heart disease, diabetes mellitus (both type 1 and type 2), obesity, smoking, obstructive sleep apnea and chronic obstructive pulmonary disease (COPD). The crude prevalence is lower in non-Western countries, primarily due to the younger age-composition in those countries (adjusted prevalence figures are scarce). The overall prevalence in a Western population is 1.0% to 1.5%. Approximately 10% of individuals aged 80 years and above have atrial fibrillation, whereas the arrhythmia is unusual among persons younger than 50 years of age. Prevalence of atrial fibrillation correlates strongly with age.
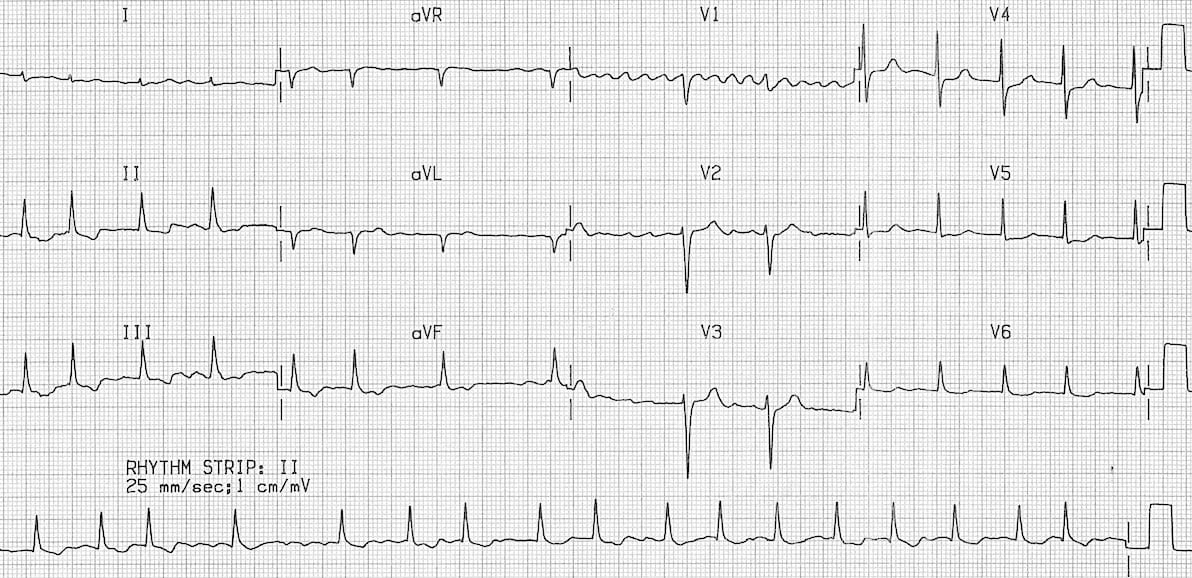
Atrial fibrillation: definitions, causes, risk factors, ECG diagnosis and managementĪtrial fibrillation is the most common pathologic tachyarrhythmia (only sinus tachycardia is more common).
